 Research shows increasing your intake of fresh fruits and vegetables can boost your well-being in as little as two weeks. Although the study didn’t explain why, previous studies show eating more vegetables impacts brain, immune, and gut health — all of which affect your mood. The New Zealand study divided more than 170 young adults into three groups. The researchers personally gave one group two servings on fresh fruits and vegetables each day. The second group was given vouchers and text reminders to consume extra produce. The third group was not given any produce or vouchers. The first group given the extra produce in person consumed an average of 3.7 servings a day of fruits and vegetables. After two weeks they reported feeling improvements in mood, vitality, motivation, as well as a flourishing of well-being. The other two groups reported no change. 5 ways eating more produce makes you feel better When you look at the effects of a plant-based diet on health, the results of this study are no surprise. Here are five reasons why eating more fruits and vegetables can make you happier and more motivated: Eating more vegetables increases the gut bacteria that promotes relaxation. Brain scans show healthy gut bacteria promotes relaxation. Eating more vegetables increases the gut bacteria that lower brain inflammation. A Harvard-affiliated study found that healthy gut bacteria lowers brain inflammation, thus lowering the risk of dementia. Brain inflammation is also linked with depression, anxiety, and irritability. Eating more vegetables increases the gut bacteria that lower depression, anxiety, eating disorders, autism symptoms, and obesity. By now you get the picture. Studies continue to find links between gut bacteria and a variety of mood and mental disorders. Eating a wide variety of plenty of produce is the best way to create a healthy diversity of gut bacteria. Regular bowel movements from increased fiber of a high-vegetable diet improve your mood. It’s no mystery why constipated babies are so fussy. Research shows a higher prevalence of mood disorders in those with chronic constipation. Although myriad factors can cause constipation, often it’s as simple as too little plant fiber. Eating ample amounts of vegetables and fruits promotes regular, healthy bowel movements (unless you have a gut disorder that makes digesting produce difficult). Constipation increases circulating toxins in the body, which can inflame the brain and leads to bad moods. What does a serving of vegetables look like? The new recommendation from the American Institute for Cancer Research is to eat at least five servings a day of fruits and vegetables, but ideally you should eat seven to ten. Five of those servings should be vegetables and two to three fruit (to avoid consuming too much sugar). In other words, two-thirds of each meal should be vegetables. A “serving” is a vague reference. Here are some ideas of what a serving looks like:
Pre-prep veggies for quick salads, and make big batches of veggie soups and stews to facilitate the transition. A few quick snack ideas:
0 Comments
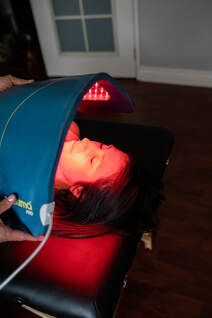 I treat a lot of patients who are dealing with thyroid issues - primarily hypothyroidism. But what I frequently find is that hypothyroidism is only a symptom of a larger problem, often some type of chronic autoimmune disorder like Hashimoto’s, which causes inflammation of the thyroid, leading to symptoms like weight gain, fatigue, joint and muscle pain, constipation, difficulty getting pregnant, and joint and muscle pain. Thyroiditis is commonly treated with a synthetic form of the thyroid stimulating hormone, but a study shows that 10 sessions of Low Level Light Therapy (LLLT) may provide anti-inflammatory effects which can increase thyroid function. Many patients who did 10 sessions of LLLT were not only able to stop taking their thyroid medication but the LLLT actually helped to regenerate damaged thyroid tissue. If you’re suffering from hypothyroidism due to a chronic autoimmune disorder like Hashimoto’s, Well Balanced Body is pleased to offer Low Level Light Therapy treatment. Ten sessions are recommended in order to see the full effects of this treatment. You can now book your light therapy sessions online! 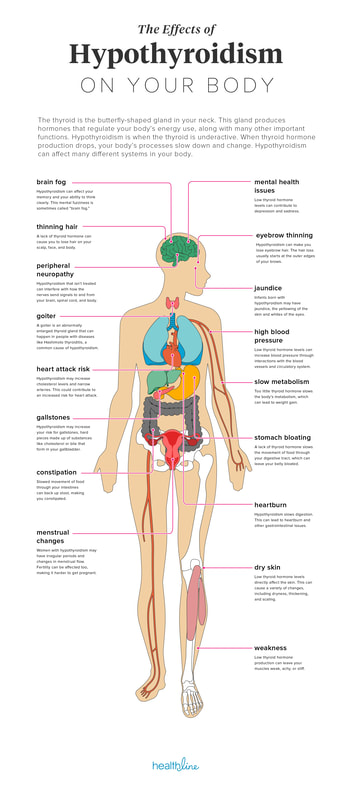 There has been an uptick in online attention around hypothyroidism since the publication of Why Do I Still Have Thyroid Symptoms? by Datis Kharrazian in 2009. While many facets should be addressed in managing hypothyroidism, one of the most important continues to be a gluten-free diet. Research shows ninety percent of hypothyroidism cases are due to an autoimmune disease that attacks and destroys the thyroid gland. This disease is called Hashimoto’s. Most doctors do not test for Hashimoto’s because it does not change treatment, which is thyroid medication. Also, many cases of hypothyroidism go undiagnosed because Hashimoto’s can cause the lab marker TSH to fluctuate. Where does gluten fit in with this? Numerous studies have linked an immune reaction to gluten with Hashimoto’s hypothyroidism. Whether it’s a gluten sensitivity or celiac disease, gluten triggers an autoimmune attack on the thyroid gland in many people. Most of these people do not even know they are sensitive to gluten. Going off gluten is the first step with Hashimoto’s Studies, clinical observation, and patient stories make a very strong case for the benefits of going gluten-free to better manage your Hashimoto’s hypothyroidism symptoms. A number of studies for several countries show a link between Hashimoto’s and gluten. This is because the protein structure of gluten closely resembles that of thyroid tissue. When your immune system reacts to gluten, it may start erroneously reacting to thyroid tissue as well. This will cause the immune system to attack and destroy thyroid tissue in a case of mistaken identity. Studies also show patients improve on a strict gluten-free diet. One study showed as many as 71 percent of subjects resolved their hypothyroid symptoms after following a strict gluten-free diet for one year. Why you may need to stop eating other foods too Sorry to say, going gluten-free alone doesn’t always work. Many people with Hashimoto’s hypothyroidism also need to go dairy-free. Dairy, whether it’s cow, goat, or sheep, is the second biggest problem food for people with Hashimoto’s hypothyroidism. Many people simply have an immune intolerance to dairy and aren’t aware of it until they stop consuming it. However, in an immune sensitive individual, the body may also mistake dairy for gluten and trigger an immune reaction that ultimately ends up targeting the thyroid. For those serious about managing their Hashimoto’s hypothyroidism, a gluten-free and dairy-free diet frequently results in profound alleviation of symptoms, if not total remission. Many find they may need to eliminate additional foods, such as certain grains, eggs, or soy. An elimination/provocation diet can help you figure out what your immune system reacts to, or a comprehensive food sensitivity test from Cyrex Labs. What is there left to eat? If you’re used to eating without restrictions, eliminating gluten, dairy, and possibly other foods to manage your Hashimoto’s. |
|
 RSS Feed
RSS Feed